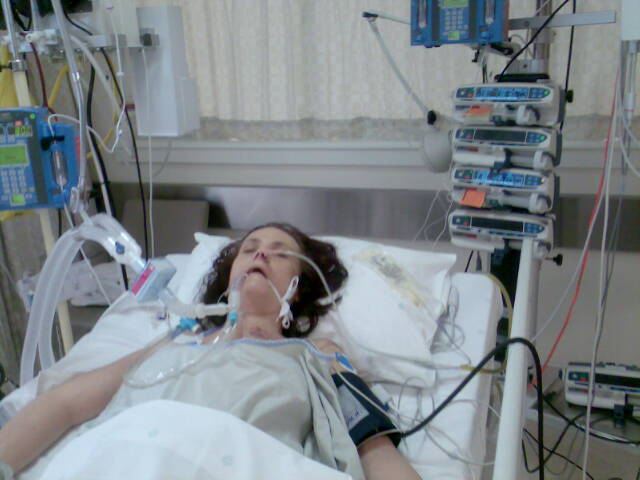
This is a subject very dear to my heart. Vic has been saved from the claws of death so many times in her little life. I often lie in bed thinking how much physical pain and discomfort I have imposed on Vic by not allowing the doctors to not give up. By cajoling her into living. Twice this week I begged her to allow me to take her to hospital. I promised earlier this year that I would respect her wishes. https://tersiaburger.com/2012/05/18/6-5-2012-3/
My BFF, Gillian, sent me this email message:
Morning, you summed up “Where did the time go” perfectly. I cannot believe that 8 years have passed so quickly. Jon Daniel was 7 and Dr said he would not understand about death, but Jared 9 would be able to comprehend and mourn. You wonder what is better……. When they are little or older. Vic our miracle child has hung in there for her Angels. She can only be commended on her will power to add another day to their lives. She has no life. Except to smile with sad eyes every time she sees the boys for another day. As hard as it is to nurse your child, you are also spared Another day good bad or ugly. God has sent Vic to us give each one a lesson – not to complain or give up – the Power of the mind. Be grateful for what we have body mind and soul. Love you all with all my heart
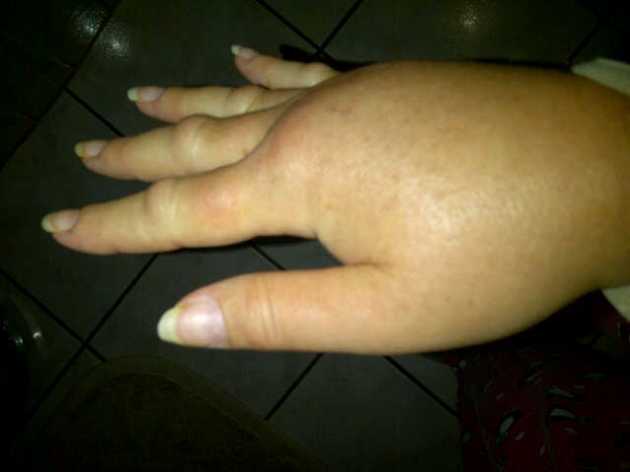
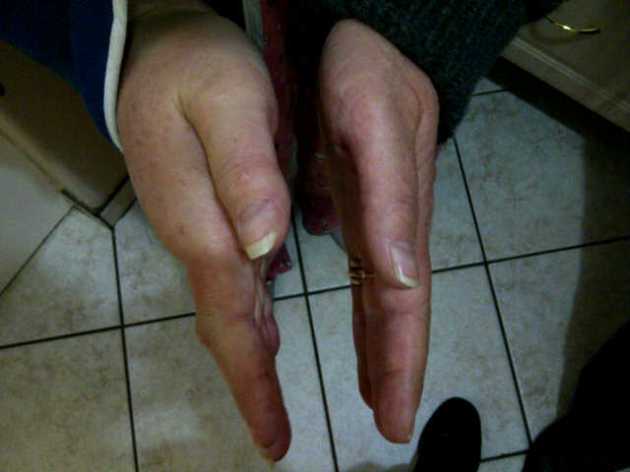
What Gillian wrote in her mail is so true. If I had allowed Vic to die earlier she would of been saved incredible amounts of raw, undiluted suffering and indignity! A couple of posts ago I wanted to include a photo of Vic’s abdomen so people could understand what a person looks like after 81 abdominal surgeries. I decided against it as it is too horrific to post. But we have been blessed with some wonderful times. The boys are now old enough to understand the extent of her suffering. At this stage I am focused on her pain. I remember when I was stressed that she was taking a couple of hundred milligrams of morphine a week. Now it is a couple of hundred per day…
Reblogged from http://www.kevinmd.com/blog/2012/11/life-discussion-important.html by JANICE BOUGHTON, MD on November 11th, 2012 in PHYSICIAN. I read this on Andrew’s blog on http://lymphomajourney.wordpress.com/2012/11/15/an-end-of-life-discussion-is-one-of-the-most-important-to-do-right/
During an internal medicine residency, newly hatched doctors are responsible for some of the sickest patients in their teaching hospitals. This is because those patients often don’t have private doctors to attend them and are poor and sometimes self abusive, with the complex problems that go with smoking, drug and alcohol abuse and lack of regular medical care. These patients often present with their diseases late in game, when much must be done quickly.
There is little or no time to discuss end of life issues and so the assumption is made that these folks want “everything done” which includes machines and potions to support organs and bodily functions as they cease to work right. A scenario might look like this: 48 year old heroin abuser comes in with fever of 104 and symptoms of a stroke. He is admitted to the intensive care unit with low blood pressure, becomes gradually delirious and his heart rate increases, he is sedated for trying to crawl out of bed and run off, he becomes lethargic and is unable to breathe for himself, a central line is inserted and he is intubated and put on a ventilator, his blood pressure is supported with pressors and fluids, his oxygen level cannot be supported despite high ventilator settings. His kidneys cease to work and his heart goes into a rhythm that produces no blood pressure at all, he receives CPR with chest compressions, he is resuscitated, but barely alive, unable to communicate, obviously brain damaged beyond repair, placed on dialysis, eventually succumbs to overwhelming infection. We call this a “flail.” It is horrifying and time consuming and ultimately a colossal waste of human and monetary resources. Repeated experiences of this type sour most of us on the idea of being resuscitated, so many doctors consider themselves “DNR (do not resuscitate).” We don’t want to be resuscitated ever, no matter what. There are some things that are worse than death.
Some resuscitations go well, though. A patient arrives in the emergency department with chest pain, develops an arrhythmia, has chest compressions briefly and electrical cardioversion and is conscious within minutes or hours. Some people briefly can’t support their own needs for respiration and require a few days of ventilation before being able to breathe adequately. Although they are weak and puny for awhile, they go home and live to tell the story, go back to work, raise families, climb mountains. These successes usually happen to people who were vital before they became really sick, the younger folks, without multiple or terminal illnesses to begin with.
When someone is admitted to the hospital, the physician responsible for their care (which is more and more often the hospitalist) determines, if possible what their wishes would be regarding life support should their breathing or heart stop. These discussions are very difficult if the patient has not thought about resuscitation and has not talked with a physician who knows them about options.
Often patients have reasonable hesitance to make potentially life determining decisions with a doctor who they don’t know and who doesn’t have time to talk with them about the implications of these decisions. In our heads we have a pretty good idea of which patients would do well should they require cardiopulmonary resuscitation, and we really want people whose chances of recovery are lousy to tell us that they are DNR. A DNR decision means that will not flail them. We will not get into a situation in which failure is likely. Should this patient become so sick that medicines, hydration and appropriate surgical procedures cannot save them, we will transition to a strategy that makes death peaceful and painless.
We rarely succeed in communicating this to patients and many who will not benefit from cardiopulmonary resuscitation say “Oh yes, doctor, I want everything done.” Some say this because their experiences are different from ours, they have seen doctor shows in which resuscitation was successful, they think that withholding resuscitation means getting substandard care, and sometimes they think that we just want to spare ourselves the trouble of saving them. And some of these concerns are valid. A patient who is “DNR” may not be watched as closely or treated as quickly if they decompensate. Some people with horrible prognoses do get better after being resuscitated, though this is pretty uncommon and usually involves a pretty significant decrement in quality of life.
Even though it is hard to establish trust with patients or their families in the context of being a hospitalist, I think it is one of the most important discussions to do right. It is everso tricky, though. Even asking the question can make a patient frightened or hostile. They wonder if we are asking this question because we secretly think they are going to die soon. They feel that the subject is too private to broach with a near stranger. They have never thought about it and don’t want to start now. They think that if they make a decision not to be resuscitated that their family members will think that they don’t love them.
But sometimes patients have been waiting, oh so patiently, for someone to bring up the subject and be willing to take enough time to answer the questions that they have been afraid to ask. I find that a discussion of resuscitation is best started after I learn about who a patient is and what they have done for a living and what they spend their time doing at home. What were they good at when they worked? Do they have kids or grandkids? Where do they live, do they travel, do art, take care of other people, have pets? It is hard or impossible to help a person navigate the end of life if I don’t know them.
Even though I am a bit biased against intensive and technological medical care, I love actually doing it. The tools of this trade are really clever and the immediacy of the practice is inspiring and brings people together. I have seen beautiful and compassionate intensive care, which makes patients and families feel valued. Nevertheless, there are always the unintentional and casual cruelties of disturbed sleep, needles, boredom, prickly heat, bowel indignities, physical pain and nausea. Death following chest compressions and electrical cardioversion is not peaceful.
When I sit with a person and hear that, no, they don’t want intensive care or cardiopulmonary resuscitation should their heart or lungs cease to work, and it is clear that resuscitation is not in their best interest, my heart feels lighter. I can focus more on what the patient values rather than what procedures are most likely to keep them alive for the longest time.
Janice Boughton is a physician who blogs at Why is American health care so expensive?