There are times in the life of a terminally ill person that death is no longer the enemy but rather a friend. Vic too surpassed all anniversaries and eventually I though she was invincible. But with invincibility comes pain, indignity, despair, depression… Thinking of you Mike in your brave journey.
Tag: pain control
We need a miracle again….
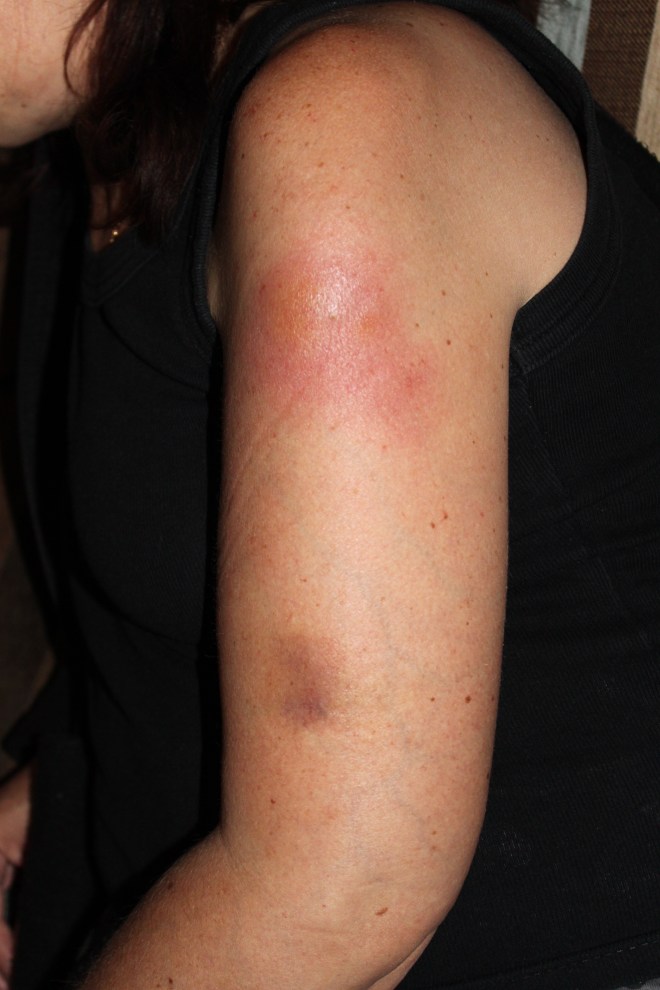
Sr Siza examined Vic today. She phoned Dr Sue who will be in tomorrow morning. She also brought a script with for Dalacin antibiotics. The cellulitis has spread to all three the subcutaneous sites.
Siza expressed her concern at Vic’s decline…
Last Friday Danie, my husband, came and sat next to me and said “I know everyone says it will be better for Vic to die than live in this pain but I was thinking how hard it will be for us without her…”
That statement really shook me. Up until now death has been a hypothetical issue… Doctors diagnoses and prognosis…predictions… I have never really considered living without my child.
Last week Siza and I met with the CEO of Amcare, a large community project that provide community based feeding schemes, HIV/AIDS Counselling, Home-based care, skills development, ARV Clinic, women and children shelters. We are hoping that they will “host” our Hospice at their premises.
The CEO knows Vicky and the boys. Jared was confirmed in his church earlier this year.
I shared with them how difficult it was to get a terminally ill person into a Hospice Program and that 95% of the dying population die in pain. Vernon (CEO) quietly listened to us and explained how difficult fundraising is. Christians are tight with their money…
Vernon then shared the following with us.
“In 2007 I was driving home from a meeting when I felt this urgent need to see Vicky. I knew she was in hospital as she was on the prayer list. I drove to the Donald Gordon (Hospital) and was directed to the ICU. The nurses welcomed me although it was way past visiting time.”
“Pray for her. We are switching the machines off tomorrow morning…” they said.
“I stood next to her bed, raised my arms and prayed that God would spare Vicky for her little boys. I stood next to a dead person that night. Two days later I heard that Vicky did not die when the machines were turned off…”
I just stared at him. I was speechless… I had no idea! It was the first time I had ever heard the story!
In June 2007 Vic had developed ARDS (Acute Respiratory Distress Syndrome) after a series of operations trying to close up an abdominal fistula. Her body was excreting up to 7 litres of faecal matter a day and she had every superbug the ICU could offer. On the Tuesday Vic went into respiratory failure and was ventilated. I was talking to her when the doctors rushed us out of ICU and put her onto the ventilator. By the Thursday her kidneys and liver had started shutting down.
ARDS is a severe lung syndrome (not a disease) caused by a variety of direct and indirect issues. It is characterized by inflammation of the lung parenchyma leading to impaired gas exchange with concomitant systemic release of inflammatory mediators causing inflammation, hypoxemia and frequently resulting in multiple organ failure. This condition is often fatal, usually requiring mechanical and admission to an intensive care unit. http://en.wikipedia.org/wiki/Acute_respiratory_distress_syndrome
My BFF, Gillian drove 350 kilometres to be with me. On the Thursday there was absolutely no sign that Vic could or would recover. Vic had a DNR and a living will that she had provided the hospital.
That evening one of the ICU doctors, Liam, hugged me and said “Mommy, Vic is tired. You must let her go…”
Gill, Leeann (Vic’s friend) and I went home after visiting hour to talk to the boys. They were already in bed when we arrived home. We sat with them
“Guys, you know how ill Mommy has been….Mommy’s lungs are not able to work on their own. Mommy’s kidneys and liver is also not working that well anymore. The doctors feel that Mommy will not be able to breathe without the machines and that Mommy has suffered too much. They think it will be better for Mommy to be taken off the machines…”
Jared quietly started to cry. Jon-Daniel was stoic. Jared was 10 years old and Jon-Daniel 8 years old.
“What will happen with us Oumie” Jon-Daniel asked.
“Sweetie, Oumie and Oupie will ALWAYS be here for you. This is your home.”
Jared cried himself to sleep. Jon-Daniel just clung to me. The three of us shared a bed that night.
The next morning early Gill, Lee and I set off to hospital. When we arrived I said “I am not going into that hospital until I have prayed in the Chapel.”
The three of us prayed and it was with absolute certainty that I KNEW Vic would not die that day.
Family and friends drifted in and out of the waiting room the whole day. My minister came and prayed for my child. Everyone said goodbye.
That afternoon Danie and I were allowed to see Vic. The “invasive” ventilator had been disconnected and she had a mask-like ventilator covering her face. It was a grotesque sight.
Danie held her little hand and his tears dripped onto her arm.
“Oh sweetie” he said, the sorrow and pain raw in his voice.
Vic opened her eyes and said “Daddy”….
Three days later Vic was discharged from ICU….. It was not her time.
Today I looked at her and fear struck at my heart. My child is slowly slipping away. Her little body is tired of the pain. Her little organs are enlarged and diseased. Her bones weak….
And the realisation hit home…. We need another miracle.
God please have mercy on my child.
Where to now?
The subcutaneous driver is down. By this morning it was obvious that Vic’s tissue was just not holding up.
On Friday morning I removed and repositioned the driver. Serum leaked out of the syringe hole for almost two days. The area is inflamed, hot to the touch, swollen and painful. Cellulitis has struck! Yesterday evening I repositioned the driver again and this afternoon I removed it. So I will now administer the 150mg of morphine and the 60 ml Stemitil IM. Vic’s derriere is black and blue and lumpy from the injections.
Where to from here? How are we going to control this poor child’s pain? I can only think that they will have to fit a central line… Will they do it? She will have to go into theatre for that! There is absolutely no way I would allow the procedure without sedation! Central lines are very susceptible to infection and sepsis.
Poor baby. She is so ill.
Today I said to my BFF, Gillian, that it is almost as if, now the decision has been made regarding “her” Hospice, she is at peace. I sat next to her and thought to myself “I wonder if she will make Christmas?” But then I thought to myself “Wait a minute…This is Vic…She bounces back!”
Tomorrow her doctor will come and see her, she will go onto a course of antibiotics and bounce back again. Then we will decide how to deal with her pain…
Central venous catheter http://en.wikipedia.org/wiki/Central_venous_catheter
| Central venous catheter | |
|---|---|
| Intervention | |
| MeSH | D002405 |
In medicine, a central venous catheter (“central line”, “CVC”, “central venous line” or “central venous access catheter”) is acatheter placed into a large vein in the neck (internal jugular vein), chest (subclavian vein or axillary vein) or groin (femoral vein). It is used to administer medication or fluids, obtain blood tests (specifically the “mixed venous oxygen saturation”), and directly obtain cardiovascular measurements such as the central venous pressure.
Contents[hide] |
Types
There are several types of central venous catheters:[1]
Non-tunneled vs. tunneled catheters
Non-tunneled catheters are fixed in place at the site of insertion, with the catheter and attachments protruding directly. Commonly used non-tunneled catheters include Quinton catheters.
Tunneled catheters are passed under the skin from the insertion site to a separate exit site, where the catheter and its attachments emerge from underneath the skin. The exit site is typically located in the chest, making the access ports less visible than if they were to directly protrude from the neck. Passing the catheter under the skin helps to prevent infection and provides stability. Commonly used tunneled catheters include Hickman catheters and Groshong catheters.
Implanted port
A port is similar to a tunneled catheter but is left entirely under the skin. Medicines are injected through the skin into the catheter. Some implanted ports contain a small reservoir that can be refilled in the same way. After being filled, the reservoir slowly releases the medicine into the bloodstream. An implanted port is less obvious than a tunneled catheter and requires very little daily care. It has less impact on a person’s activities than a PICC line or a tunneled catheter. Surgically implanted infusion ports are placed below the clavicle (infraclavicular fossa), with the catheter threaded into the right atrium through large vein. Once implanted, the port is accessed via non-coring “Huber” needles inserted through the skin. The health care provider may need to use topical anesthetic prior to accessing port. Ports can be used for medications, chemotherapy, TPN, and blood. As compared to CVC or PICC catheters, ports are easy to maintain for home-based therapy.
Ports are typically used on patients requiring only occasional venous access over a long duration course of therapy. Since the port must be accessed using a needle, if venous access is required on a frequent basis a catheter having external access is more commonly used.
PICC line
A peripherally inserted central catheter, or PICC line (pronounced “pick”), is a central venous catheter inserted into a vein in the arm rather than a vein in the neck or chest.
Technical description
Depending on its use, the catheter is monoluminal, biluminal or triluminal, dependent on the actual number of lumens (1, 2 and 3 respectively). Some catheters have 4 or 5 lumens, depending on the reason for their use.
The catheter is usually held in place by an adhesive dressing, suture, or staple which is covered by an occlusive dressing. Regular flushing with saline or a heparin-containing solution keeps the line patent and prevents thrombosis. Certain lines are impregnated with antibiotics, silver-containing substances (specifically silver sulfadiazine) and/or chlorhexidine to reduce infection risk.
Specific types of long-term central lines are the Hickman catheters, which require clamps to make sure the valve is closed, and Groshong catheters, which have a valve that opens as fluid is withdrawn or infused and remains closed when not in use. Hickman lines also have a “cuff” under the skin, to prevent bacterial migration[citation needed] and to cause tissue ingrowth into the device for long term securement.
Indications and uses
Indications for the use of central lines include:[2]
- Monitoring of the central venous pressure (CVP) in acutely ill patients to quantify fluid balance
- Long-term Intravenous antibiotics
- Long-term Parenteral nutrition especially in chronically ill patients
- Long-term pain medications
- Chemotherapy
- Drugs that are prone to cause phlebitis in peripheral veins (caustic), such as:
- Calcium chloride
- Chemotherapy
- Hypertonic saline
- Potassium chloride
- Amiodarone
- vasopressors (e.g. epinephrine, dopamine)
- Plasmapheresis
- Peripheral blood stem cell collections
- Dialysis
- Frequent blood draws
- Frequent or persistent requirement for intravenous access
- Need for intravenous therapy when peripheral venous access is impossible
Central venous catheters usually remain in place for a longer period of time than other venous access devices, especially when the reason for their use is longstanding (such as total parenteral nutrition in a chronically ill patient). For such indications, a Hickman line, a PICC line or a portacath may be considered because of their smaller infection risk. Sterile technique is highly important here, as a line may serve as a porte d’entrée (place of entry) for pathogenic organisms, and the line itself may become infected with organisms such as Staphylococcus aureus and coagulase-negative Staphylococci.[citation needed]
The skin is cleaned, and local anesthetic applied if required. The location of the vein is then identified by landmarks or with the use of a small ultrasound device. A hollow needle is advanced through the skin until blood is aspirated; the color of the blood and the rate of its flow help distinguish it from arterial blood (suggesting that an artery has been accidentally punctured), although this method is inaccurate.[citation needed] Ultrasound probably now represents the gold standard for central venous access and skills, within North American and Europe, with landmark techniques are diminishing.[3][4]
The line is then inserted using the Seldinger technique: a blunt guidewire is passed through the needle, then the needle is removed. A dilating device may be passed over the guidewire to slightly enlarge the tract. Finally, the central line itself is then passed over the guidewire, which is then removed. All the lumens of the line are aspirated (to ensure that they are all positioned inside the vein) and flushed.[citation needed] A chest X-ray is typically performed afterwards to confirm that the line is positioned inside the superior vena cava and, in the case of insertion through the subclavian vein, that no pneumothorax was caused as a side effect. Vascular positioning systems can also be used to verify tip placement during insertion without the need to a chest X-ray, but this technique is not yet a standard of practice.
Videos are available demonstrating placement of a central venous catheter without[5] and with ultrasound guidance.[6]
Complications
Central line insertion may cause a number of complications. The benefit expected from their use therefore needs to outweigh the risk of those complications.
Pneumothorax
Pneumothorax (for central lines placed in the chest); the incidence is thought to be higher with subclavian vein catheterization. In catheterization of the internal jugular vein, the risk of pneumothorax can be minimized by the use of ultrasound guidance. For experienced clinicians, theincidence of pneumothorax is about 1.5-3.1%. Some official bodies, e.g. the National Institute for Health and Clinical Excellence (UK), recommend the routine use of ultrasonography to minimize complications.[7]
Central-Line Associated Bloodstream Infections (CLABSIs)
All catheters can introduce bacteria into the bloodstream, but CVCs are known for occasionally causing Staphylococcus aureus andStaphylococcus epidermidis sepsis. The problem of central line-associated bloodstream infections (CLABSI) has gained increasing attention in recent years. They cause a great deal of morbidity and deaths, and increase health care costs. Historically, a small number of CVC infections were considered an acceptable risk of placing central lines. However, the seminal work by Dr. Peter Pronovost at Johns Hopkins Hospital turned that perspective on its head. Additionally, the Institute for Healthcare Improvement (IHI) has done a tremendous amount of work in improving hospitals’ focus on central line-associated bloodstream infections (CLABSI), and is working to decrease the incidence of this particular complication among US hospitals.
The National Patient Safety Goals NPSGs and specifically NSPG 7.04 address how to decrease infections.[8] The NSPG 7.04 has 13 elements of performance to decrease CLABSIs.
The 13 Elements of Performance (EPs):
- EP 1 & 2 deal with educating staff and patients about Central Vascular Catheters and their potential complications
- EP 3 specifically directs facilities to implement policies and practices to reduce CLABSI
- EP 4 & 5 are about how to perform surveillance for Central-Line Associated Bloodstream Infections (CLABSIs)
- EP 6-13:
– Institute for Healthcare Improvement (IHI) bundle
- 1. Hand Hygiene
- 2. Full body drape
- 3. Chlorhexidine gluconate skin anti-septic
- 4. Selection of Optimal site for Central venus Catheter (CVC)
- 5. Daily review of ongoing need for CVC
– Disinfection of intravenous access ports before use
National Patient Safety Goals require documentation of a checklist for CVC insertion and Disinfection of intravenous (IV) access ports before use (scrub the hub). Some literature has suggested the use of a safer vascular access route – such as intraosseous (IO) vascular access – when central lines are not absolutely necessary (such as when central lines are being placed solely for vascular access). Infection risks were initially thought to be less in jugular lines, but this only seems to be the case if the patient is obese.[9]
If a patient with a central line develops signs of infection, blood cultures are taken from both the catheter and from a vein elsewhere in the body. If the culture from the central line grows bacteria much earlier (>2 hours) than the other site, the line is the likely source of the infection. Quantitative blood culture is even more accurate, but this is not widely available.[10]
Generally, antibiotics are used, and occasionally the catheter will have to be removed. In the case of bacteremia from Staphylococcus aureus, removing the catheter without administering antibiotics is not adequate as 38% of such patients may still develop endocarditis.[11]
In a clinical practice guideline, the American Centers for Disease Control and Prevention recommends against routine culturing of central venous lines upon their removal.[12]The guideline makes a number of further recommendations to prevent line infections.[12]
To prevent infection, stringent cleaning of the catheter insertion site is advised. Povidone-iodine solution is often used for such cleaning, but chlorhexidine appears to be twice as effective as iodine.[13] Routine replacement of lines makes no difference in preventing infection.[14]
Thrombosis
CVCs are a risk factor for forming venous thrombosis[15] including upper extremity deep vein thrombosis.[16]
Other complications
Rarely, small amounts of air are sucked into the vein as a result of the negative Intra-thoracic pressure and insertion technique. Valved insertion devices can reduce this risk.[citation needed] If these air bubbles obstruct blood vessels, this is known as an air embolism.
Hemorrhage (bleeding) and formation of a hematoma (bruise) is slightly more common in jugular venous lines than in others.[9]
Arrhythmias may occur during the insertion process when the wire comes in contact with the endocardium. It typically resolved when the wire is pulled back.[citation needed]
Morphine extends life!

The downward pain spiral has already begun. Vic is quite swollen and had a bad day. This afternoon late she perked up and has only had one vomiting spell tonight.
As Sr Siza was examining her this afternoon and taking her vitals I remarked on the swelling. “It’s the organs shutting down” she whispered….
“I am scared Siza. I administer such massive dosages of medication to Vic… What if I kill her?” I asked over a cup of tea.
“Don’t worry my love. You won’t. There is no upper limit to the amount of morphine that Vicky can go on… As long as we titrate the dosages she will be fine.”
So I Googled Morphine+dosage+death and one of the first articles that came up (and I could understand) is “When Morphine Fails to Kill” By GINA KOLATA
Proponents of assisted suicide often argue that when a doctor helps a patient who wants to die, it is no more ethically troubling than when a doctor kills a patient slowly with morphine, often without the patient’s knowledge or consent, a medical practice these proponents say is increasingly common.
So why forbid doctors to prescribe lethal pills that could allow patients to control how and when they die? There is no question that doctors use morphine this way. “It happens all the time,” said Dr. John M. Luce, a professor of medicine and anesthesiology at the University of California in San Francisco. And there is no question that most doctors think that morphine can hasten a patient’s death by depressing respiration. But Luce and others are asking whether morphine and similar drugs really speed death.
Experts in palliative care say the only available evidence indicates that morphine is not having this effect. Dr. Balfour Mount, a cancer specialist who directs the division of palliative care at McGill University in Montreal, firmly states that it is “a common misunderstanding that patients die because of high doses of morphine needed to control pain.”
No one denies that an overdose of morphine can be lethal. It kills by stopping breathing. But, said Dr. Joanne Lynn, director of the Center to Improve Care of the Dying at George Washington University School of Medicine, something peculiar happens when doctors gradually increase a patient’s dose of morphine. The patients, she said, become more tolerant of the drug’s effect on respiration than they do of its effect on pain. The result, Dr. Lynn said, is that as patients’ pain gets worse, they require more and more morphine to control it. But even though they end up taking doses of the drug that would quickly kill a person who has not been taking morphine, the drug has little effect on these patients’ breathing.
Dr. Kathleen Foley, who is co-chief of the pain and palliative care service at Memorial SloanKettering Cancer Center in New York, said that she routinely saw patients taking breathtakingly high doses of morphine yet breathing well. “They’re taking 1,000 milligrams of morphine a day, or 2,000 milligrams a day, and walking around,” she said.
The standard daily dose used to quell the pain of cancer patients, she added, is 200 to 400 milligrams. Dr. Lynn said she sometimes gave such high doses of morphine or similar drugs that she frightened herself. She remembers one man who had a tumor on his neck as big as his head. To relieve his pain, she ended up giving him 200 milligrams of a morphinelike drug, hydromorphone, each hour, 200 times the dose that would put a person with no tolerance to the drug into a deep sleep. “Even I was scared,” Dr. Lynn said, but she found that if she lowered the dose to even 170 milligrams of the drug per hour, the man was in excruciating pain. So to protect herself in case she was ever questioned by a district attorney, she said, she videotaped the man playing with his grandson while he was on the drug.
On rare occasions, Dr. Lynn said, she became worried when she escalated a morphine dose and noticed that the patient had started to struggle to breathe. Since she did not intend to kill the patient, she said, she administered an antidote. But invariably, she said, she found that the drug was not causing the patient’s sudden respiratory problem.
One man, for example, was having trouble breathing because he had bled from a tumor in his brain, and an elderly woman had just had a stroke. “In every single case, there was another etiology,” Dr. Lynn said. “Joanne’s experience is emblematic,” said Dr. Russell K. Portenoy, the other cochief of the pain and palliative care service at Memorial SloanKettering Cancer Center.
He said he was virtually certain that if doctors ever gave antidotes to morphine on a routine basis when dying patients started laboring to breathe, they would find that Dr. Lynn’s experience was the rule. Patients generally die from their diseases, not from morphine, Dr. Portenoy said.
The actual data on how often morphine and other opiates that are used for pain relief cause death are elusive. But Dr. Foley and others cite three studies that indirectly support the notion that if morphine causes death, it does so very infrequently. One study, by Dr. Frank K. Brescia of Calvary Hospital in the Bronx and his colleagues, examined pain, opiate use and survival among 1,103 cancer patients at that hospital, which is for the terminally ill. The patients had cancer that was “very far advanced,” said Dr. Portenoy, an author of the paper. But to his surprise, he said, the investigators found no relationship between the dose of opiates a patient received and the time it took to die. Those receiving stunningly high doses died no sooner than those taking much lower doses.
Another study, by Dr. Luce and his colleagues in San Francisco, looked at 44 patients in intensive care units at two hospitals who were so ill that their doctors and families decided to withdraw life support. Three quarters of the patients were taking narcotics, and after the decision was made to let them die, the doctors increased their narcotics dose. Those who were not receiving opiates were in comas or so severely brain damaged that they did not feel pain. The researchers asked the patients’ doctors to tell them, anonymously, why they had given narcotics to the patients and why they had increased the doses. Thirty nine (39%) percent of the doctors confided that, in addition to relieving pain, they were hoping to hasten the patients’ deaths. But that did not seem to happen.
The patients who received narcotics survived an average of 3 1/2 hours after the decision had been made to let them die. Those who did not receive narcotics lived an average of 1 1/2 hours. Of course, Dr. Luce said, the study was not definitive because the patients who did not receive drugs may have been sicker and more likely to die very quickly. Nonetheless, he said, the investigators certainly failed to show that narcotics speeded death.
Dr. Declan Walsh, the director of the Center for Palliative Medicine at the Cleveland Clinic, said it had been 15 years since he first questioned the assumption that morphine used for pain control killed patients by depressing their respiration. He was working in England at the time, and many doctors there were afraid to prescribe morphine or similar drugs for cancer patients, Walsh said, because “they were afraid they would kill the patients.”
So Walsh looked at carbon dioxide levels in the blood of cancer patients on high doses of morphine to control their pain. If their breathing was suppressed, their carbon dioxide levels should have been high. But they were not. Nonetheless, Walsh said, the idea that morphine used for pain relief depresses respiration is widely believed by doctors and nurses because it is “drummed into them in medical school.” So, said Dr. Susan Block, a psychiatrist in the hematology and oncology division at Brigham and Women’s Hospital in Boston, it is not surprising that many doctors try to use morphine to speed dying. “There is more and more evidence most of it unpublished, but it’s coming, I’ve seen it that physicians, in addition to wanting to ease patients’ discomfort, also want to hasten death,” Dr. Block said. “Everyone is feeling guilty.”
Source: NY TIMES July 23, 1997 http://www.chninternational.com/Opiods%20for%20pain%20do%20not%20kill.htm
No more pain angel.
Signposts for Dying
Yesterday I posted on “time”. Today after the visit from the Hospice sister I actually realized that just maybe Vic has entered the first stages of dying
Some of the stages of dying start to be discernible a few months before death occurs.
Vic has become less active; she rests more, sleeps more and has withdrawn into her own inner realm.
Vic is reliving memories and spends a lot of her awake time talking to the boys about her childhood, her “illustrious” school career and their childhoods. This year she relived every minute of her father’s final journey… Vic has started living in the past.
I read that it is the terminally ill’s way of taking stock of their lives and making their peace with it.
Vic no longer eats big meals and I seldom hear her say “I am ravenous”. Due to the 81 abdominal surgeries and multiple bouts of septicemia Vic’s absorption is very poor. (Poor absorption = BIG appetite!) Vic used to have the appetite of a horse – always nibbling and scrounging for food. Now it is sheer discipline that keeps her eating. She knows she cannot have medication without eating first. Strange thing is that she is not really losing weight. Hospice says it is due to the high levels of cortisone she takes… I have been told by Hospice not to worry about her loss of appetite. Her body does not need a lot of fuel (food) anymore because it is not burning a lot of energy anymore….
The effect of the reduced food and liquid intake is that the body starts producing chemicals that create a feeling of mild euphoria. Our bodies actually start relaxing into this stage of dying.
Vic still drinks a fair amount of coffee. She used to drink it warm but now she dozes off before she has finished her cup of coffee. She will wake up and take a sip of cold coffee… A cup of coffee now lasts a long time.
Vic spends the majority of the day in bed, gently dozing…. It is not a deep sleep. It is as if her little body is preparing to hibernate….preparing for what lies beyond death whether it is Heaven, Nirvana or the Other Side….
Reduced appetite and increased sleep is called “Signposts for dying”.
A couple of weeks ago Vic was very emotional. She would tear up without any reason. This stage has passed. It is as if her tears cleansed her soul.
Vic is battling with loneliness. She hates being alone. If she could she would have one of us around her all the time. She often complains that we do not spend time with her. We do spend a lot of time with her. She just dozes off and then we leave to carry on with our lives… The boys are writing exams – they have to study; I have to work…. Dying is a lonely journey
Vic is not in good shape at all. She is suffering severe cramping and nausea that is not responding to any of the medication. The Hospice Sister called the doctor this afternoon and asked her to see Vic in the morning. She also suggested that Vic be admitted to Hospice In-Patient’s. Vic and I firmly declined…
It is obvious that Vic has one or other infection. I think it is the abdominal sepsis. She seems flushed and feels hot and cold. The thermometer does not reflect her running a fever. This is obviously something as Ceza mentioned it to the doctor. She explained that this happens when the auto-immune system is compromised. I have tried to Google it but without too much success. I will ask the doctor tomorrow morning.
Vic is in terrible pain tonight. I have already given her double her normal evening morphine injections; double the quantity of morphine syrup; I have changed her Durogesic patches…. I lay behind her back and gently held her until her breathing became deep and even. She whimpered in her drug-induced sleep….
I know the shutting down process has started. Not because Hospice told me but because Vic told me.
Will my poor baby’s hell ever end? If there is a lesson to be learnt PLEASE God show me what it is so I can learn it!! This has come to an end!
“How did it get late so soon” – Dr Seuss

Today I read a lovely blog that Andrew had reblogged. http://lymphomajourney.wordpress.com/2012/11/10/living-with-cancer-its-about-time-nytimes-com/
Several studies have suggested that when dealing with terminal illnesses, especially cancer, doctors are usually incorrect in their prognosis, nearly always tending to believe that their patients will live longer than they actually do.
In one study involving patients in Chicago hospice programs, doctors got the prognosis right only about 20 % of the time, and 63% of the time overestimated their patients’ survival.
Interestingly, the longer the duration of the doctor-patient relationship, the less accurate was the prognosis. “Disinterested doctors . . . may give more accurate prognoses,” the authors wrote, “perhaps because they have less personal investment in the outcome.” http://www.kevinmd.com/blog/2012/04/doctors-incorrect-prognosis-terminal-illness.html
Eight years ago we were told that Vic’s life was “compromised” and that she would die within the next 5 years. Eight years later Vic is still alive. Maybe Vic’s doctor is too close to Vic….
Eleven years ago Vic had blotched back surgery setting her off on a journey filled with pain, 81 abdominal surgeries, years in hospital and millions of rands worth of medical expenses.
Vic realized that her life had been compromised and started saying “If only I can see Jared go to school…” I remember her joy the first day Jared went to school. Then she said “If only I can live to see Jon-Daniel go to school…” I remember how desperately ill she was the day Jon-Daniels started school….
Now both her boys are in High School. I never hear Vic saying “I wish” anymore.
Tonight we discussed going to the coast for a week in January. Vic just shook her head sadly and said “It is too far Mommy. Even if I fly down I think it will be too much for me…”
It is all about time.
Time grinds to a halt when Vic needs her 4 hourly pain medication and there is an hour to go… when she screams from pain and her blood pressure is too low for more pain medication to be administered…
The longest nights are the nights before surgery and after surgery. The longest passage is the passage outside the operating theater and ICU.
Whilst I was in the UK Vic did well. She fired her nurse and administered her own injections into her legs! I have been home for six days and Vic is really ill. I expected her to have the “up-time” whilst I was gone. I knew that she would use every ounce of her residual strength to be “good” while I was gone. Vic bounced around and amazed everyone who came into contact with her. Cr Ceza, her Hospice sister, however spoke to her in the presence of Danie and Esther and told her that the ONLY reason she was feeling great was because her pain control was optimal. Her body would however betray her. She said that Vic’s body has started shutting down….slowly but surely. The process is inevitable… I believe that Hospice is wrong. They have to be wrong.
Tonight I am sitting here just wondering where time has gone.
The Blog I read today articulated my thoughts and emotions so accurately!
“In the immortal words of Dr. Seuss, “How did it get so late so soon?” Without much of a future, surely time will again change. A lot can happen in a year — think of the helpless infant becoming a walking, talking toddler in 9 or 10 months. Time moves more slowly for small children, since a year of a 2-year-old’s life is 50 percent of that life. A terminal diagnosis may also slow down time. The next year might be 100 percent of what’s left of my existence.”
Sometimes the time left seems too long; too many catastrophes could injure those I love. Sometimes it seems too short; there are so many suspenseful stories unfolding around me, and I want to see how they will turn out. Those for whom time’s chariot is indeed winged often attest to a heightened appreciation of their fast-fading prospects. And then there is always the dream of borrowed time, that numinous period beyond the predicted end, like a stay of execution, which must be fraught with its own blessings and curses. . http://lymphomajourney.wordpress.com/2012/11/10/living-with-cancer-its-about-time-nytimes-com/
We have already had so many “extra” years. But the fact remains that Vic is ill. Today she is more ill than yesterday or even last week or last month. It is not an UTI causing the pain and fever. Her pain control is good enough to mask symptoms. Waves of severe nausea and cramping remain…
I don’t even want to consider the possibility that the pain is caused by Vic’s organs slowly starting to shut down….. One organ after another…. I have read that it feels “uncomfortable”. It is called terminal agitation.
Only time will tell…. Time is all we have….
How did it get late so soon?
Related Posts:
https://tersiaburger.com/2012/10/15/remission-15-10-2012/https://tersiaburger.com/2012/08/02/5-stages-of-dying/ https://tersiaburger.com/2012/08/08/dummys-guide-for-the-parents-of-a-terminally-ill-child/
https://tersiaburger.com/2012/07/02/vic-regrets-not-going-to-italy/ https://tersiaburger.com/2012/07/20/thank-you-god-20-7-2012/ https://tersiaburger.com/2012/08/05/what-can-we-hope-for-when-there-is-no-hope/
“Being prepared to die is one of the greatest secrets of living.” George Lincoln Rockwell
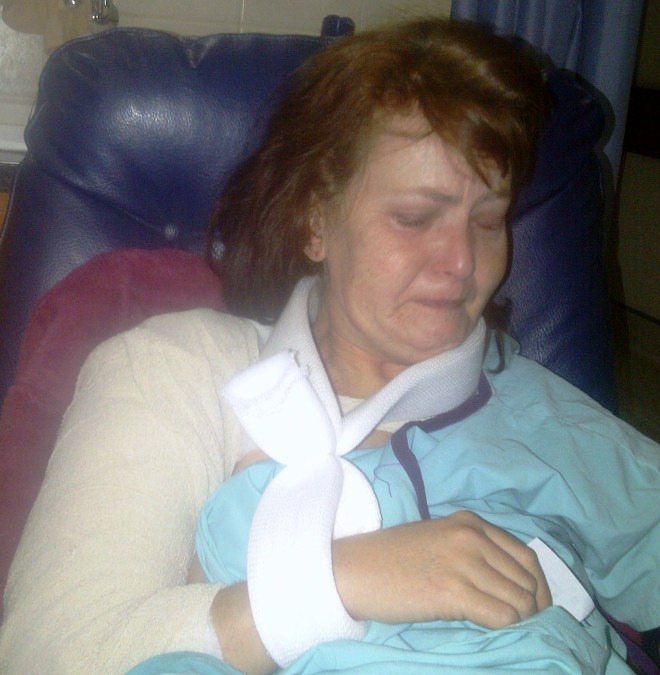
Pain at the end of life is inescapably interwoven with, and often amplified by, multiple levels of emotional and spiritual angst as the inevitability of death looms. Fear, a potent pain magnifier, is the dominant emotion – fear of pain, fear of death, fear of the unknown…..
It is a fact that people at the end of life fear pain even more than they fear death. Sadly, for many dying patients, pain seems like the ultimate torment, and death is its cure. It does not have to be this way, and if you or a loved one is facing death, you have every right to ask that your final days not be consumed by pain.
It is estimated that a maximum of 5% of people who die from terminal illness in South Africa have access to adequate palliative care. Even in hospitals, treatment is far from ideal, because doctors and nurses have seldom had training in palliative care and have little idea of what to do with the patients.
Dying patients are often prey to a host of anxieties about the state of their affairs, about the fate of those who will grieve their loss, and about how their behaviour will be seen, and possibly judged, during their final hours. And of course, there are often deep spiritual and religious questions to address. Did my life have meaning? Will my soul survive my body? Am I at peace with myself, my family, and my friends?
Not least of all these concerns, people at the end of life worry about how their pain will be managed. Will they be under medicated and have to ask, or even beg for relief? Will they be over-medicated and lose consciousness during their precious waning days and hours?
They may even be afraid to complain. If they do, will they be seen as whiners or quitters? If they ask for narcotics, will they be judged by their doctors as drug seeking, drug addicts or even cowardly? Or will their medical care be relegated to comfort measures only, while all efforts to cure their illness are suspended?
I read the post of an amazing woman who is suffering from congenital heart failure. She is in so much pain. I cried when I read her post. http://thedrsays.org/2012/11/08/ She replied to a question whether better pain control was possible….. “there is nothing that will let me participate in life and have relief. so at this point i am going for being lucid over some so-so pain relief. who knows how long before i cave. when the time comes i plan to take advantage of whatever is available to me. just my personal choice right now.”
Vic has received a new lease on life. Vic has 100% better quality of life since her pain is under control. We discovered, through the expertise of a wonderful palliative care team that Vic’s body did not absorb monstrous quantities of morphine! Now she is not only functioning, she is LIVING! Vic is more lucid than she was before.
The pain was killing Vic… Palliative care has given her life.

 Being prepared to die is one of the greatest secrets of living.
Being prepared to die is one of the greatest secrets of living.  George Lincoln Rockwell
George Lincoln Rockwell
WebMD Pain Coach
I found this wonderful ap and would like to share it with you. Hope this is someone out there that may find this useful!! Well done Apple!
WebMD Pain Coach
By WebMD http://www.webmd.com/mobile
Description
WebMD Pain Coach™ offers a holistic approach to balancing lifestyle with chronic pain conditions to help inspire a better day. WebMD’s new app is a mobile companion to help you through daily health and wellness choices so you can better manage your chronic pain. Enjoy a personalized experience as physician-reviewed tips related to your specific condition are delivered daily to you. WebMD Pain Coach™ puts you in control of your lifestyle choices so you can review personal patterns to understand triggers, set goals, and easily share progress with your physician.
WebMD Pain Coach™ is specially designed and customized for people with the following chronic pain conditions:
✓ Back pain
✓ Neck pain
✓ Nerve pain
✓ Fibromyalgia
✓ Migraine
✓ Osteoarthritis
✓ Rheumatoid arthritisIf your chronic pain condition is not listed above, you can still use the app to track pain, set goals, and get pain management tips, articles, slideshows and videos.
When you first download and use WebMD Pain Coach™, you are asked to select your chronic pain condition(s), as well as symptoms, triggers and treatments that apply to your condition(s). If privacy is important, the option to set a four digit PIN will keep your information secure. WebMD’s drug look-up allows you to search and select over-the-counter and prescribed medications, and record the dosage of each drug selected.
WebMD Pain Coach™ is organized into four easy-to-use sections:
✓ JOURNAL
The Journal section allows you to quickly and easily record your day. A separate Journal screen exists for each day. Once entries are created for multiple days, flip back to see your pain history. Turn your phone sideways to generate your Pain Coach™ Report: a historical chart that plots your general well-being against your pain levels while listing your most common symptoms, triggers and treatments. Tap on a day to view a snapshot of your pain history and export your Pain Coach™ Report to PDF and email it to yourself or your physician.
♦ Record how you generally feel each day by sliding the Pain Coach™ ‘Well Being Belt.’
♦ Log a pain entry to track details surrounding pain: pain level from 1-10, symptoms, triggers, treatments and notes.
♦ Reminder to log a pain entry by receiving a Pain Coach™ notification once a day.
♦ View a new Daily Tip that is personalized to your condition(s), triggers and treatments.
♦ If you set goals to better manage pain, tap ‘Today’s Goals’ to check off achieved goals.✓ Goals
The Goals section allows you to browse and select physician-approved goals from five lifestyle categories related to your pain condition(s): Food, Rest, Exercise, Mood, and Treatments. You can also create your own goals. Each related tip can be viewed before selecting a goal. The goal duration can be set from one day to one year.
♦ The green ribbon at the top of the Goals screen indicates the percent completion rate for active goals.
♦ Once a goal is selected, tap ‘My Goals’ to view Goal Activity for active and completed goals.
♦ If you have more than one chronic pain condition, the goal that is suggested for a specific condition is indicated.✓ Library
The Library section contains all of the critical, physician-approved content relevant to your condition(s) and pain management. The Library contains hundreds of articles, videos, slideshows and quizzes. All articles are available for offline reading.
♦ Library content contains links to WebMD’s mobile website.
♦ The Library is searchable.
♦ Share all Library content via email, Facebook or Twitter.✓ Tips
The Tips section features hundreds of ‘bite-sized’ tips that are matched with goals and organized into the same five lifestyle categories: Food, Rest, Exercise, Mood and Treatments. Each goal has between 3-10 supporting tips.
♦ Search for a specific tip.
♦ After reading a tip, view the goal related to the tip, or view related Library articles.iPhone Screenshots
Customer Reviews
Great app
by Dragon Slayer 1
What a game changer. I can finally define my pain in my terms.
brilliant app!
by pyroclasticlux
excellent for tracking my migraines & other chronic pain. it’s a well thought-out app & is very user-friendly! i definitely recommend this programme; it is both easy to use and comprehensive.
Great little app for my neck pain
by Grimlock2011
On a recent ride to Cheyenne i bit it and was in the hospital for 2 days. Some disks popped in my neck, and let me tell you, goody’s powder wasn’t cutting it. i like this app because it helps me think about ways to feel better and i can also show my doctor my pain charts. looking foward to rejoining the boys and riding again soon! Get this app you won’t be sorry.
Remission 15.10.2012

On the 17th of September Vicky was accepted onto the Hospice program. Dr Sue Walters, the Hospice doctor and Sr Ceza, Hospice Nursing Sister, thought she would die within days. Vic was barely conscious and too weak to walk. Vic was breathing but had already ceased to live!
In two days’ time we celebrate Vic’s “One Month with Hospice” and I think she is getting stronger every day. We still have bad days but her pain control is great! Vic is reasonably mobile; she laughs and spends constructive time with the boys and the family! She is sorting out photos and all sorts of things that she has neglected for months. She is spending less time in bed. She is sleeping less and eating more.
It is as if she has a new lease on life!
Could it be possible that the pain was killing her? Is it possible that the adhesions have stopped their devastating path of destruction? That just maybe the sepsis has cleared?
Vic still needs assistance with basics. Vic could live like this. We could live like this. Please let this continue! Today I pray that this is the case. I pray for a miracle. I pray that Vic is in remission.
Remission (medicine), the state of absence of disease activity in patients with a chronic illness, with the possibility of return of disease activity. http://en.wikipedia.org/wiki/Remission
Palliative care

Today, having a loved one live with a terminal diagnosis for an extended period of time is fast replacing sudden and unexpected death as the norm. Ultimately, many will reach a point where medical technology may be able to keep them alive but can neither restore their health nor even improve their condition. In actual fact they are merely kept breathing…. More treatment will only prolong their dying.
It is at this point that patients and families face difficult choices about the kind of care they want….
I have seen studies that clearly show that patients who access Hospice, earlier in the disease process, actually live longer than expected. Ironically it seems that Hospice, with its emphasis on quality of life, actually keeps people going. When people who are ill have good pain and symptom control and their caregivers are well supported, they don’t want to give up; they want to live longer.
Vic has reached a stage in her life where she wants to die. She has absolutely no quality of life and is growing weaker by the day. Everyday Vic loses a little more of her independence and dignity. Vic needs help with almost all her day-to-day activities.
Opinion polls decisively show that most people would prefer to die at home, free from pain and surrounded by their loved ones. Sadly people often die alone in hospitals or nursing homes, attached to life support machines they do not want. It is also a fact thatmany terminally ill people die excruciating painful deaths because, even in death, their doctors suffer from Opiophobia…
“Opiophobia is the syndrome of failure to administer adequate opioid analgesics because of the fear of producing addiction or toxicity. The etiology of opiophobia is multifactorial: Peer pressure (provider and patient), regulatory agency pressure (real or perceived), and lack of education on opioids and the fundamentals of pain management all contribute to its persistence…. All of these factors contribute to the underuse of these relatively simple and very effective medications, due to no fault of the patients. ” University of Wisconsin textbook on pain medicine, Bonica’s Management of Pain, 3rd edition:
I promised Vic no more surgery and no more hospitals. https://tersiaburger.com/2012/06/01/1-6-2012 The only humane option left is Hospice. I have been fighting for Hospice to get involved with Vic’s palliative care not to hasten her death but to enhance her quality of life!
WHAT IS PALLIATIVE CARE
Palliative care is an approach that improves the quality of life of patients and their families facing the problem associated with life-threatening illness, through the prevention and relief of suffering by means of early identification and impeccable assessment and treatment of pain and other problems, physical, psychosocial and spiritual. Palliative care:
- provides relief from pain and other distressing symptoms;
- affirms life and regards dying as a normal process;
- intends neither to hasten or postpone death;
- integrates the psychological and spiritual aspects of patient care;
- offers a support system to help patients live as actively as possible until death;
- offers a support system to help the family cope during the patients illness and in their own bereavement;
- uses a team approach to address the needs of patients and their families, including bereavement counselling, if indicated;
- will enhance quality of life, and may also positively influence the course of illness;
- is applicable early in the course of illness, in conjunction with other therapies that are intended to prolong life, such as chemotherapy or radiation therapy, and includes those investigations needed to better understand and manage distressing clinical complications. http://www.hospicepalliativecaresa.co.za/What_is_palliative_care.html
WHAT TO EXPECT
Should the patient be accepted onto a hospice programme, the Hospice team together with the patient will develop a tailor-made plan care plan. Usually patients are visited by the hospice staff in their own homes. The care and support of the hospice team will help the patient and family as they navigate their way through the challenges of living with a life-limiting condition.
The main things hospice can help with are:
- pain and symptom control
- psycho-social support and advise
- spiritual support
- emotional support
- bereavement support
- equipment (wheelchairs etc)
The challenges that we as a family must face with Vic’s terminal diagnosis is complex. It includes evolving new structures and dynamics as the person we love very, very slowly slips away.
Last night and again tonight, Vic said to me “Mommy, I know you think I will live forever but you must prepare yourself because I know how my body feels…”
As a family we have learnt to cope with setbacks, Vic’s health steadily deteriorating and periods of seeming remission. This “extended grief”, wears us down and leads to the horrible realization that we sometimes find ourselves wishing that the process would end…. I have often said “Sometimes I am scared Vic will never die…” I do not want my child to die. I merely want her suffering to END!
As a family we have moved into a phase where the stress of the situation can no longer be ignored. It is making all of us ill.
This week has been an emotional roller coaster! On Tuesday I cried in front of a strange doctor. Wednesday I felt that I was losing the plot. I was unable to function on a professional level. My mind was absolutely fogged over. Thursday an angel named Christa evaluated Vic and I went from absolute despair to exuberance when I heard that Hospice’s Doctor would evaluate Vic on Monday morning…
Today when Jared and I were waiting to see the doctor after his CT scan we had a long chat…
He said “Oumie I can see when you are stressed. You zone out… You have been very stressed this week….”
“Yeah” I said. “I have been a little stressed this week.”
“Since you starting writing your blog you no longer wear a mask Oumie…You handled the stress better before! You always smiled.”
OMG. What am I doing to the boys? I realized today that I have to be more careful. The mask has to go back on. I scare them when I show my stress. Imagine what it would do to them if they read my blog….. Thank God they don’t!
I left the best for last though – no immediate lymph biopsy will be done on Jared. The lymph nodes are definitely enlarged but there has been no adverse change in the past two and a half weeks. We will give his kidney some time to heal and the CT scan will be repeated again in two months time.
I am feeling so positive!
There is a God and I thank him for Jared’s outcome, Hospice intervention, Baby Isak and my wonderful, loving family. I pray that He will enfold Vic and the boys in His Mercy and Grace. I pray for my mask!
September and awareness of pain
As a mother of a terminally ill child, who suffers debilitating chronic pain, I have researched pain extensively. I have argued with physicians and meet with pain specialists at the pain clinic every month. I have bullied hospital nursing staff. I have witnessed and lived my child screaming like a wounded animal from pain….. Doctors telling her that she is a morphine addict and pharmacists double-checking and verifying Vic’s scripts…
September and awareness of pain.
Dummy’s Guide for the Parents of a Terminally ill Child
Dummy’s Guide for the Parents of a Terminally ill Child

I often read about a child that had been ill for a long time and the parent being in denial. Death is never discussed. I know it may take months or even years for Vic to die. Maybe, with a bit of luck, I will die before she does. But when either one of us dies there will be nothing unspoken. Vic and I talk a lot. We talk about many things. If ever I think of something that I am not certain of, I ask her immediately.
I have fully accepted that Vicky is always walking the tightrope even when she is doing great. It is the nature of the beast and the beast can take you by surprise.
We have spoken about heaven and what a peaceful, healthy place it will be. We often speak about meeting again in heaven and Vic always says she is not scared of dying. Vicky feels terrible about leaving us behind. She worries about leaving us all behind. She worries about how sad we will be. I wish I knew what to say to truly put her mind at peace and to let her “let go”…
It was very difficult to first raise the question of death. It started approximately 8 years ago with a tentative “Sweetie, is all your paperwork in order before you have this surgery?” and progressed to discussing and shopping for 18th birthday gifts, Confirmation bibles and 21st Birthday Keys. It was strangely “pleasant” going shopping with Vic. I knew that her mind was at ease having done the shopping. Maybe she will be around for these milestone events. Maybe not….. But Vic is prepared. She is far more prepared than I am. She has written letters to be read after her death. She has “special events” cards that I will give the boys when the occasion or need arises.
To arrive at the point, where we are, has been hell! No matter what age your child is, when you first find out that your child is terminally ill, your initial instinct is to shelter the child. (Regardless of the child’s age – the child will always remain the child!!) The parent’s first instinct is to leave no stone unturned. You watch the child like a hawk, looking for small signs of improvement or deterioration, looking for symptoms, hoping against all hope that the doctor made a mistake!
I analyze every ache and pain, hoping that the stomach cramps are merely side effects of the medication. I know when Vic is heading for a UTI; I know how her body reacts to different medications. Unfortunately there is no “Dummy’s Guide for the Parents of a Terminally ill Child”.
Professional counselling is available at a terrible cost. By the time your child is diagnosed or rather sentenced to terminal illness, hundreds and hundreds of thousands of rands has been spent on medical bills. Within two months of the new medical year the medical aid is exhausted….. The medication and treatment cannot stop regardless of the claimable amount left on the medical aid limits… I have said it before – morphine or counselling???? No contest! Morphine wins hands down. Now in a civilized world Hospice should enter the picture at this stage….. Unfortunately we live in South Africa and Vic does not have AIDS or cancer. I pray that she will find the peace that I know she does not have.
No-one in the world can live in so much pain for so long!
It has to end sometime.
What can we hope for when there is no hope?
What can we hope for when there is no hope?
 When Brendan (Vic’s gastroenterologist) took me into the passage, outside Vic’s hospital room, and said “No more. This is the end of the road” my heart stopped. How can there be no hope? Brendan has been so brave until that moment. It was not easy for him to sentence Vic to the “No Hope” section of her journey.
When Brendan (Vic’s gastroenterologist) took me into the passage, outside Vic’s hospital room, and said “No more. This is the end of the road” my heart stopped. How can there be no hope? Brendan has been so brave until that moment. It was not easy for him to sentence Vic to the “No Hope” section of her journey.
Where does hope live when we hear the words announced to us, “There is no hope”? We cannot return to life as it was.
Immanuel Kant, who lived and wrote in the 1700s, thought a lot about the kind of subjects we might label as “the eternal verities”: hope, ethics, God, morality, the meaning of life. Kant came up with three questions that he thought expressed the central human concerns. Here are his famous questions:
What can I know?
What can I do?
What can I hope?
What can I know?
“A large part of Kant’s work addresses the question “What can we know?” The answer, if it can be stated simply, is that our knowledge is constrained to mathematics and the science of the natural, empirical world. It is impossible, Kant argues, to extend knowledge to the super sensible realm of speculative metaphysics. The reason that knowledge has these constraints, Kant argues, is that the mind plays an active role in constituting the features of experience and limiting the mind’s access only to the empirical realm of space and time.” http://www.iep.utm.edu/kantmeta/
I know I can only address this on an emotional level.
I know that life is unfair and difficult! I know we are scared – not only of Vic’s painful journey but of what lies beyond her release from pain. I know I hate seeing my child suffer and losing her dignity.
I know I love my child more than life. I know she wants to live. I know she wants to love, be loved….. I know she wants the frustration of facing peak hour traffic on her way to work or back. I know Vic wants a job. I know Vic wants financial independence, a trip to Italy. I know Vic wants to attend her sons 21st Birthday parties, see them graduate, and meet the person they decide to spend their lives with. Hold her grandchild..…grow old gracefully. I know Vic wants to walk on the beach, see the sun set over the sea…..
I know that Vic is tired of the pain. I know she wants to die. I know she wants to live.
I know dying is a lonely journey. I know it is impossibly difficult to watch Vic grow weaker every day. I know I am tired of being sad. I know I want the boys to be happy…..
What should I do?
I know I should honor Vic’s wishes. I know that I should try and stay positive for the boys sake. I should fight harder for Hospice intervention. I should remain cheerful and snap out of my depression. I should concentrate on the positive moments in our lives. I should endeavor to find a way of giving Vic peace – enough peace to let go.
What can I hope?
I wish her pain control will continue to work as well as it is now… I hope that her suffering will come to an end. I hope that the boys will heal in time. I hope that we will laugh again. I hope that Vic will find peace.
I hope that my beautiful little girl will fall asleep and not wake up. I hope that God will be with her when the time comes