Sr Siza examined Vic today. She phoned Dr Sue who will be in tomorrow morning. She also brought a script with for Dalacin antibiotics. The cellulitis has spread to all three the subcutaneous sites.
Siza expressed her concern at Vic’s decline…
Last Friday Danie, my husband, came and sat next to me and said “I know everyone says it will be better for Vic to die than live in this pain but I was thinking how hard it will be for us without her…”
That statement really shook me. Up until now death has been a hypothetical issue… Doctors diagnoses and prognosis…predictions… I have never really considered living without my child.
Last week Siza and I met with the CEO of Amcare, a large community project that provide community based feeding schemes, HIV/AIDS Counselling, Home-based care, skills development, ARV Clinic, women and children shelters. We are hoping that they will “host” our Hospice at their premises.
The CEO knows Vicky and the boys. Jared was confirmed in his church earlier this year.
I shared with them how difficult it was to get a terminally ill person into a Hospice Program and that 95% of the dying population die in pain. Vernon (CEO) quietly listened to us and explained how difficult fundraising is. Christians are tight with their money…
Vernon then shared the following with us.
“In 2007 I was driving home from a meeting when I felt this urgent need to see Vicky. I knew she was in hospital as she was on the prayer list. I drove to the Donald Gordon (Hospital) and was directed to the ICU. The nurses welcomed me although it was way past visiting time.”
“Pray for her. We are switching the machines off tomorrow morning…” they said.
“I stood next to her bed, raised my arms and prayed that God would spare Vicky for her little boys. I stood next to a dead person that night. Two days later I heard that Vicky did not die when the machines were turned off…”
I just stared at him. I was speechless… I had no idea! It was the first time I had ever heard the story!
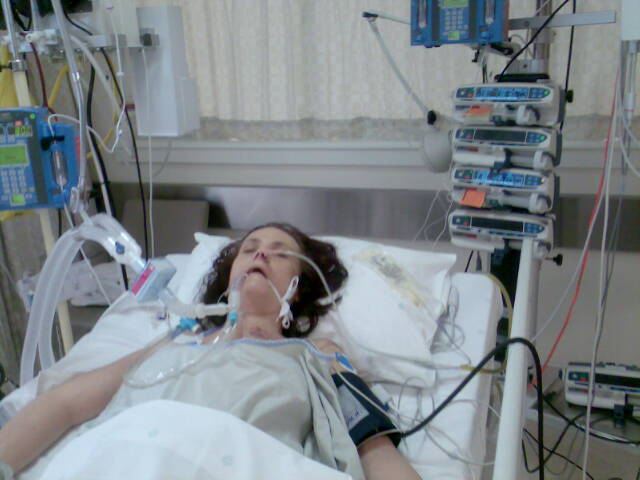
In June 2007 Vic had developed ARDS (Acute Respiratory Distress Syndrome) after a series of operations trying to close up an abdominal fistula. Her body was excreting up to 7 litres of faecal matter a day and she had every superbug the ICU could offer. On the Tuesday Vic went into respiratory failure and was ventilated. I was talking to her when the doctors rushed us out of ICU and put her onto the ventilator. By the Thursday her kidneys and liver had started shutting down.
ARDS is a severe lung syndrome (not a disease) caused by a variety of direct and indirect issues. It is characterized by inflammation of the lung parenchyma leading to impaired gas exchange with concomitant systemic release of inflammatory mediators causing inflammation, hypoxemia and frequently resulting in multiple organ failure. This condition is often fatal, usually requiring mechanical and admission to an intensive care unit. http://en.wikipedia.org/wiki/Acute_respiratory_distress_syndrome
My BFF, Gillian drove 350 kilometres to be with me. On the Thursday there was absolutely no sign that Vic could or would recover. Vic had a DNR and a living will that she had provided the hospital.
That evening one of the ICU doctors, Liam, hugged me and said “Mommy, Vic is tired. You must let her go…”
Gill, Leeann (Vic’s friend) and I went home after visiting hour to talk to the boys. They were already in bed when we arrived home. We sat with them
“Guys, you know how ill Mommy has been….Mommy’s lungs are not able to work on their own. Mommy’s kidneys and liver is also not working that well anymore. The doctors feel that Mommy will not be able to breathe without the machines and that Mommy has suffered too much. They think it will be better for Mommy to be taken off the machines…”
Jared quietly started to cry. Jon-Daniel was stoic. Jared was 10 years old and Jon-Daniel 8 years old.
“What will happen with us Oumie” Jon-Daniel asked.
“Sweetie, Oumie and Oupie will ALWAYS be here for you. This is your home.”
Jared cried himself to sleep. Jon-Daniel just clung to me. The three of us shared a bed that night.
The next morning early Gill, Lee and I set off to hospital. When we arrived I said “I am not going into that hospital until I have prayed in the Chapel.”
The three of us prayed and it was with absolute certainty that I KNEW Vic would not die that day.
Family and friends drifted in and out of the waiting room the whole day. My minister came and prayed for my child. Everyone said goodbye.
That afternoon Danie and I were allowed to see Vic. The “invasive” ventilator had been disconnected and she had a mask-like ventilator covering her face. It was a grotesque sight.
Danie held her little hand and his tears dripped onto her arm.
“Oh sweetie” he said, the sorrow and pain raw in his voice.
Vic opened her eyes and said “Daddy”….
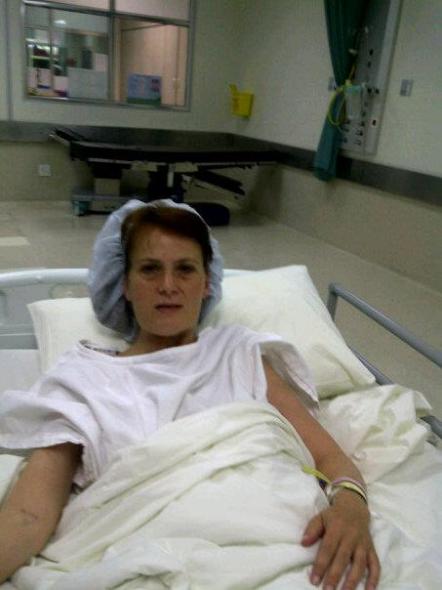
Three days later Vic was discharged from ICU….. It was not her time.
Today I looked at her and fear struck at my heart. My child is slowly slipping away. Her little body is tired of the pain. Her little organs are enlarged and diseased. Her bones weak….
And the realisation hit home…. We need another miracle.
God please have mercy on my child.