In medicine, a central venous catheter (“central line”, “CVC”, “central venous line” or “central venous access catheter”) is acatheter placed into a large vein in the neck (internal jugular vein), chest (subclavian vein or axillary vein) or groin (femoral vein). It is used to administer medication or fluids, obtain blood tests (specifically the “mixed venous oxygen saturation”), and directly obtain cardiovascular measurements such as the central venous pressure.
Types
There are several types of central venous catheters:[1]
Non-tunneled vs. tunneled catheters
Non-tunneled catheters are fixed in place at the site of insertion, with the catheter and attachments protruding directly. Commonly used non-tunneled catheters include Quinton catheters.
Tunneled catheters are passed under the skin from the insertion site to a separate exit site, where the catheter and its attachments emerge from underneath the skin. The exit site is typically located in the chest, making the access ports less visible than if they were to directly protrude from the neck. Passing the catheter under the skin helps to prevent infection and provides stability. Commonly used tunneled catheters include Hickman catheters and Groshong catheters.
Implanted port
A port is similar to a tunneled catheter but is left entirely under the skin. Medicines are injected through the skin into the catheter. Some implanted ports contain a small reservoir that can be refilled in the same way. After being filled, the reservoir slowly releases the medicine into the bloodstream. An implanted port is less obvious than a tunneled catheter and requires very little daily care. It has less impact on a person’s activities than a PICC line or a tunneled catheter. Surgically implanted infusion ports are placed below the clavicle (infraclavicular fossa), with the catheter threaded into the right atrium through large vein. Once implanted, the port is accessed via non-coring “Huber” needles inserted through the skin. The health care provider may need to use topical anesthetic prior to accessing port. Ports can be used for medications, chemotherapy, TPN, and blood. As compared to CVC or PICC catheters, ports are easy to maintain for home-based therapy.
Ports are typically used on patients requiring only occasional venous access over a long duration course of therapy. Since the port must be accessed using a needle, if venous access is required on a frequent basis a catheter having external access is more commonly used.
PICC line
A peripherally inserted central catheter, or PICC line (pronounced “pick”), is a central venous catheter inserted into a vein in the arm rather than a vein in the neck or chest.
Technical description
Depending on its use, the catheter is monoluminal, biluminal or triluminal, dependent on the actual number of lumens (1, 2 and 3 respectively). Some catheters have 4 or 5 lumens, depending on the reason for their use.
The catheter is usually held in place by an adhesive dressing, suture, or staple which is covered by an occlusive dressing. Regular flushing with saline or a heparin-containing solution keeps the line patent and prevents thrombosis. Certain lines are impregnated with antibiotics, silver-containing substances (specifically silver sulfadiazine) and/or chlorhexidine to reduce infection risk.
Specific types of long-term central lines are the Hickman catheters, which require clamps to make sure the valve is closed, and Groshong catheters, which have a valve that opens as fluid is withdrawn or infused and remains closed when not in use. Hickman lines also have a “cuff” under the skin, to prevent bacterial migration[citation needed] and to cause tissue ingrowth into the device for long term securement.
Indications and uses
Indications for the use of central lines include:[2]
Central venous catheters usually remain in place for a longer period of time than other venous access devices, especially when the reason for their use is longstanding (such as total parenteral nutrition in a chronically ill patient). For such indications, a Hickman line, a PICC line or a portacath may be considered because of their smaller infection risk. Sterile technique is highly important here, as a line may serve as a porte d’entrée (place of entry) for pathogenic organisms, and the line itself may become infected with organisms such as Staphylococcus aureus and coagulase-negative Staphylococci.[citation needed]

Triple lumen in jugular vein

Chest x-ray with catheter in the right subclavian vein
The skin is cleaned, and local anesthetic applied if required. The location of the vein is then identified by landmarks or with the use of a small ultrasound device. A hollow needle is advanced through the skin until blood is aspirated; the color of the blood and the rate of its flow help distinguish it from arterial blood (suggesting that an artery has been accidentally punctured), although this method is inaccurate.[citation needed] Ultrasound probably now represents the gold standard for central venous access and skills, within North American and Europe, with landmark techniques are diminishing.[3][4]
The line is then inserted using the Seldinger technique: a blunt guidewire is passed through the needle, then the needle is removed. A dilating device may be passed over the guidewire to slightly enlarge the tract. Finally, the central line itself is then passed over the guidewire, which is then removed. All the lumens of the line are aspirated (to ensure that they are all positioned inside the vein) and flushed.[citation needed] A chest X-ray is typically performed afterwards to confirm that the line is positioned inside the superior vena cava and, in the case of insertion through the subclavian vein, that no pneumothorax was caused as a side effect. Vascular positioning systems can also be used to verify tip placement during insertion without the need to a chest X-ray, but this technique is not yet a standard of practice.
Videos are available demonstrating placement of a central venous catheter without[5] and with ultrasound guidance.[6]
Complications
Central line insertion may cause a number of complications. The benefit expected from their use therefore needs to outweigh the risk of those complications.
Pneumothorax
Pneumothorax (for central lines placed in the chest); the incidence is thought to be higher with subclavian vein catheterization. In catheterization of the internal jugular vein, the risk of pneumothorax can be minimized by the use of ultrasound guidance. For experienced clinicians, theincidence of pneumothorax is about 1.5-3.1%. Some official bodies, e.g. the National Institute for Health and Clinical Excellence (UK), recommend the routine use of ultrasonography to minimize complications.[7]
Central-Line Associated Bloodstream Infections (CLABSIs)
All catheters can introduce bacteria into the bloodstream, but CVCs are known for occasionally causing Staphylococcus aureus andStaphylococcus epidermidis sepsis. The problem of central line-associated bloodstream infections (CLABSI) has gained increasing attention in recent years. They cause a great deal of morbidity and deaths, and increase health care costs. Historically, a small number of CVC infections were considered an acceptable risk of placing central lines. However, the seminal work by Dr. Peter Pronovost at Johns Hopkins Hospital turned that perspective on its head. Additionally, the Institute for Healthcare Improvement (IHI) has done a tremendous amount of work in improving hospitals’ focus on central line-associated bloodstream infections (CLABSI), and is working to decrease the incidence of this particular complication among US hospitals.
The National Patient Safety Goals NPSGs and specifically NSPG 7.04 address how to decrease infections.[8] The NSPG 7.04 has 13 elements of performance to decrease CLABSIs.
The 13 Elements of Performance (EPs):
- EP 1 & 2 deal with educating staff and patients about Central Vascular Catheters and their potential complications
- EP 3 specifically directs facilities to implement policies and practices to reduce CLABSI
- EP 4 & 5 are about how to perform surveillance for Central-Line Associated Bloodstream Infections (CLABSIs)
- EP 6-13:
– Institute for Healthcare Improvement (IHI) bundle
- 1. Hand Hygiene
- 2. Full body drape
- 3. Chlorhexidine gluconate skin anti-septic
- 4. Selection of Optimal site for Central venus Catheter (CVC)
- 5. Daily review of ongoing need for CVC
– Disinfection of intravenous access ports before use
National Patient Safety Goals require documentation of a checklist for CVC insertion and Disinfection of intravenous (IV) access ports before use (scrub the hub). Some literature has suggested the use of a safer vascular access route – such as intraosseous (IO) vascular access – when central lines are not absolutely necessary (such as when central lines are being placed solely for vascular access). Infection risks were initially thought to be less in jugular lines, but this only seems to be the case if the patient is obese.[9]
If a patient with a central line develops signs of infection, blood cultures are taken from both the catheter and from a vein elsewhere in the body. If the culture from the central line grows bacteria much earlier (>2 hours) than the other site, the line is the likely source of the infection. Quantitative blood culture is even more accurate, but this is not widely available.[10]
Generally, antibiotics are used, and occasionally the catheter will have to be removed. In the case of bacteremia from Staphylococcus aureus, removing the catheter without administering antibiotics is not adequate as 38% of such patients may still develop endocarditis.[11]
In a clinical practice guideline, the American Centers for Disease Control and Prevention recommends against routine culturing of central venous lines upon their removal.[12]The guideline makes a number of further recommendations to prevent line infections.[12]
To prevent infection, stringent cleaning of the catheter insertion site is advised. Povidone-iodine solution is often used for such cleaning, but chlorhexidine appears to be twice as effective as iodine.[13] Routine replacement of lines makes no difference in preventing infection.[14]
Thrombosis
CVCs are a risk factor for forming venous thrombosis[15] including upper extremity deep vein thrombosis.[16]
Other complications
Rarely, small amounts of air are sucked into the vein as a result of the negative Intra-thoracic pressure and insertion technique. Valved insertion devices can reduce this risk.[citation needed] If these air bubbles obstruct blood vessels, this is known as an air embolism.
Hemorrhage (bleeding) and formation of a hematoma (bruise) is slightly more common in jugular venous lines than in others.[9]
Arrhythmias may occur during the insertion process when the wire comes in contact with the endocardium. It typically resolved when the wire is pulled back.[citation needed]
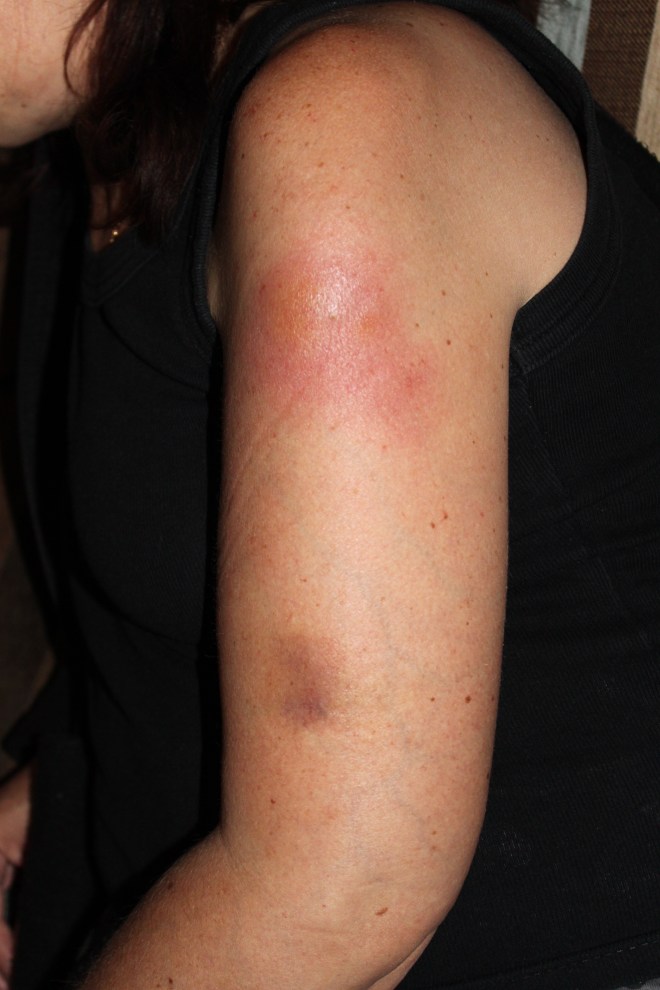
 I just finished a batch of choc-chip cookies. The house is quiet and sweet smell of the biscuits has permeated the air. The Christmas tree lights are flicking and the first batch of gifts beautifully wrapped. It is the season of Christmas. Two weeks ago I despaired that Vic would not live to see Christmas. Dr Sue came and saw Vic this morning. She lanced the cellulitis abscess on Vic’s arm. My baby girl was so brave!! Sue told us of a young man who came to see her in her rooms with a small abscess in his face. He cried with pain. Sue told Vic what a brave person she is…I was so proud of my little girl. Vic’s heart and pulse rate is very elevated. She has a kidney infection. Kidney infections make her tired. I just checked on Vic, and she is sleeping so peacefully. She has a serene expression on her beautiful face, and she is truly pain-free tonight. Sitting here I am counting my blessings. My baby girl is home. I cannot begin to imagine how difficult it would have been if Vic lived elsewhere or if she was married or involved. I can now care for my child without having to consider my “position” in her life. I am able to be her mommy and take care of her. The boys are settled and happy living with us. We love having them so close to us. They are such well-behaved, kind and helpful boys! Before Vic moved home the boys, mainly Jared, had to cook most days. Now they are able to be children. Life has settled into an easy routine. We have laughter and fun. We cry and despair. We hug. We talk and constantly affirm our love for one another. Vic is spending a lot of time with her boys – talking. She helped with the preparations for Jared’s 16th birthday party. Vic passed me the spices when I baked this year’s Christmas cakes. We laughed when we decided the cake needed another “splash of brandy”. Vic “chose” her Christmas Cake. My wonderful husband is such an amazing person. He is my rock and pillar. He loves and protects us. I am happy and content with our lives. Thank you God for this time of closeness.
I just finished a batch of choc-chip cookies. The house is quiet and sweet smell of the biscuits has permeated the air. The Christmas tree lights are flicking and the first batch of gifts beautifully wrapped. It is the season of Christmas. Two weeks ago I despaired that Vic would not live to see Christmas. Dr Sue came and saw Vic this morning. She lanced the cellulitis abscess on Vic’s arm. My baby girl was so brave!! Sue told us of a young man who came to see her in her rooms with a small abscess in his face. He cried with pain. Sue told Vic what a brave person she is…I was so proud of my little girl. Vic’s heart and pulse rate is very elevated. She has a kidney infection. Kidney infections make her tired. I just checked on Vic, and she is sleeping so peacefully. She has a serene expression on her beautiful face, and she is truly pain-free tonight. Sitting here I am counting my blessings. My baby girl is home. I cannot begin to imagine how difficult it would have been if Vic lived elsewhere or if she was married or involved. I can now care for my child without having to consider my “position” in her life. I am able to be her mommy and take care of her. The boys are settled and happy living with us. We love having them so close to us. They are such well-behaved, kind and helpful boys! Before Vic moved home the boys, mainly Jared, had to cook most days. Now they are able to be children. Life has settled into an easy routine. We have laughter and fun. We cry and despair. We hug. We talk and constantly affirm our love for one another. Vic is spending a lot of time with her boys – talking. She helped with the preparations for Jared’s 16th birthday party. Vic passed me the spices when I baked this year’s Christmas cakes. We laughed when we decided the cake needed another “splash of brandy”. Vic “chose” her Christmas Cake. My wonderful husband is such an amazing person. He is my rock and pillar. He loves and protects us. I am happy and content with our lives. Thank you God for this time of closeness.